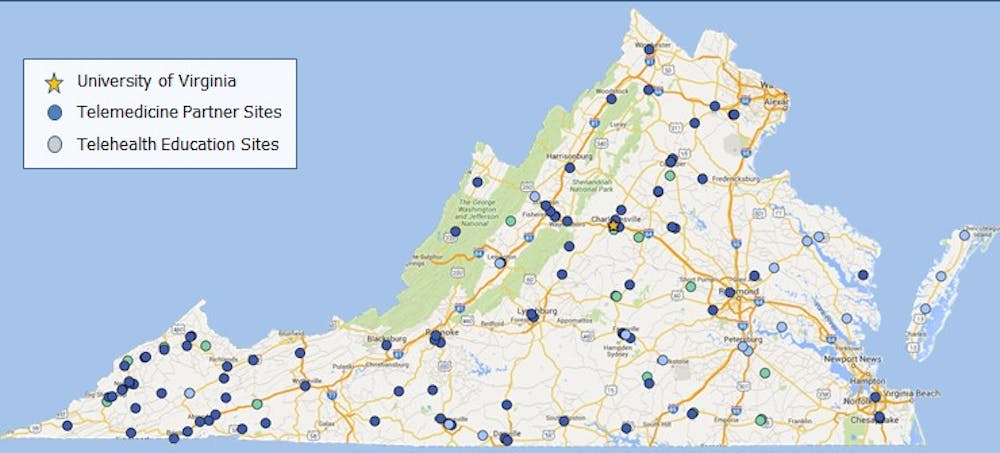
The University’s Karen S. Rheuban Center for Telehealth has saved Virginians over 16 million miles of travel in its more than two-decade history of combating disparities in the access and timeliness of healthcare.
Telemedicine is broadly defined as the use of advanced technologies to improve the quality of healthcare. It allows for remote treatment or consultation between specialists and patients or other medical providers.
The University’s Telehealth Center was co-founded 22 years ago by its namesake — Dr. Karen Rheuban, who is a pediatric cardiologist in the University Health System.
The Center now provides services in over 60 specialties and subspecialties — with 152 local partners in Virginia and 22 international programs — such as the Tanzanian Women’s Global Health Initiative and a surgical case teleconference in Rwanda.
Through the Center’s partnership with the Swinfen Charitable Trust, University Health practitioners also provide free, store-and-forward consultations for medical professionals in over 70 countries. This type of telemedicine allows practitioners to store medical images and data, send it to one of the Center’s specialists and receive feedback outside of real-time.
“There’s no billing that happens with that,” Rheuban said. “The same is true for the work we’re doing in Rwanda [and] for the work we’re doing in Uganda — this is more in support of our educational and research missions, but what we do with telemedicine is charitable here.”
The Center also provides educational services to patients and providers looking to incorporate telemedicine into their own care.
“I like to say [that] necessity is the mother of invention,” Rheuban said. “So where our patients have need, where there are workforce shortages, where we can develop partnerships with communities across the Commonwealth of Virginia and indeed other countries as well, our goal was to be there and to find creative solutions … to support that vision.”
The Office of Telemedicine, directed by David C. Gordon, oversees the clinical operations of the Telehealth Center.
Those operations run the gamut, from neonatal and high-risk obstetric services all the way to the management of chronic diseases and end-of-life care. Two of the most-used services within that spectrum are stroke care and mental health treatment, Gordon said.
Stroke neurologists at the University’s health system are able to guide partner providers in identifying the type of stroke from which a patient is suffering whether it is caused by a blocked blood vessel or ruptured vessel in the brain — and the appropriate treatment method, such as medication that would dissolve the clot-blocking the vessel.
“If you are a rural patient and you are part of our tele-stroke program, you get clot-busting medication at the same rate that you would if you were living in Charlottesville and you showed up in our emergency department for evaluation,” Rheuban said. “We’ve eliminated a lot of the disparities in access to care through the program.”
In the future, Gordon said that the Center hopes to improve upon outcomes by equipping ambulances with iPads. Through this, a stroke neurologist can assess whether or not a patient is having a stroke even before the ambulance reaches the hospital, allowing the patient to go straight into a CT scan and receive clot-busting medication faster.
“When you’re having a stroke, time is brain,” Gordon said. “If you can administer the [drug] within a set time of three hours, then you can save lives, save limbs [and] save families incredible heartache by being able to treat the patient earlier.”
Telemedicine is also well-suited to the needs of psychiatric patients, Gordon said. Since opening, the Center has had over 28,000 tele-psychiatry encounters and decreased patient no-shows by 30 percent.
“This is a tool that makes sense for mental health providers because at the core is a personal relationship, the ability to see each other and [to] have a private conversation,” Gordon said. “That’s a large part of what we do for kids, for adults [and] for emergency psych patients.”
With regards to expansion, Rheuban said that she has 90 new projects on the table and that the Center will stay involved in public policy decisions affecting patient access to telemedicine.
“One of the places that we have worked very vigorously is in developing strong public policies that support safe, high-quality telemedicine services,” Rheuban said. “[We are] working with the Medicaid agency, working with Medicare [and] working with the insurance companies to make sure that we create sustainable models of care that will continue to support this and that we do the right thing for our patients.”
Both Rheuban and Gordon said telemedicine has the potential to relieve many disparities in the access and timeliness of critical health care.
“Our goal is equivalency of care, and [it is] our belief that patients anywhere should have access to the care that they need,” Gordon said.