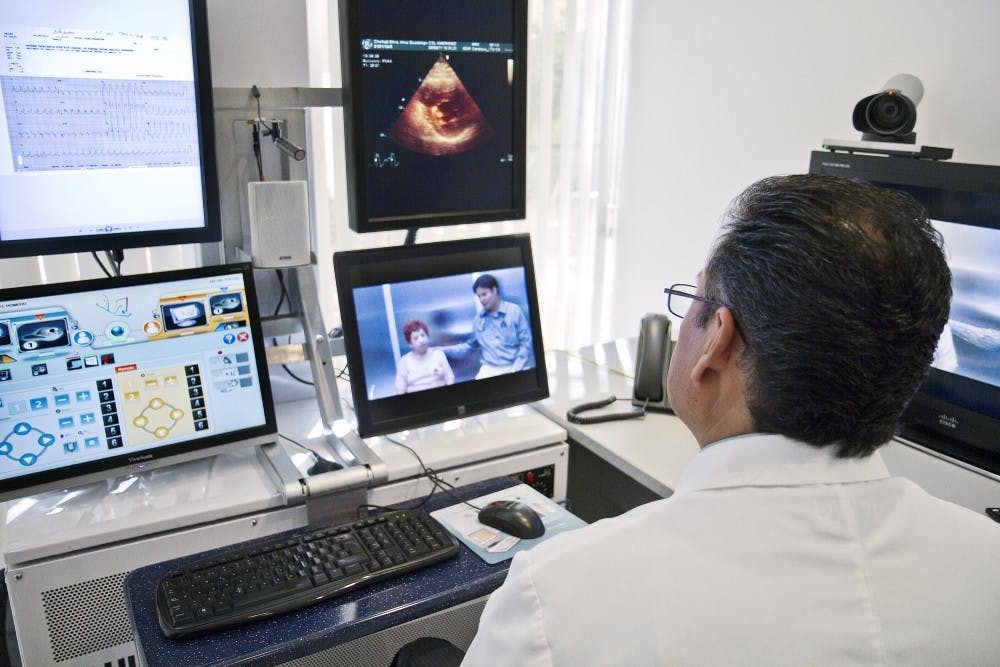
The Virginia Hepatitis Education and Patient Connection program has partnered with Medicaid, Virginia’s Department of Health and Department of Corrections to offer telemedicine services and intensive day-long training sessions for medical personnel throughout Virginia, especially those in rural areas. Rebecca Dillingham, associate professor of medicine in the Division of Infectious Diseases and Internal Health, and Terry Kemp-Knick, hepatitis C coordinator and clinical research manager of the University Health System, created this initiative to instruct clinical providers on proper hepatitis C treatment methods.
The expectation is that education and expansion of telemedicine to underserved populations in Virginia will significantly reduce, if not ultimately eradicate, hepatitis C. Dillingham said that a similar program between the University Health System and the Virginia Department of Health focused on providing assistance to those impacted by HIV in southwest Virginia. Upon realizing the prevalence of hepatitis C in these locations, the University, in collaboration with the Virginia Department of Health, decided to augment the telemedicine program to include hepatitis C patients beginning in June 2018.
“In creating that program, we prioritized partnerships with organizations that provide care for people struggling with opioid addiction,” Dillingham said. “This could be people who provide medication assisted treatment for opioid use disorder or other comprehensive harm reduction services.”
Training sessions first launched a year later in June 2019 and are now held once every three months. These workshops allow doctors, physicians assistants and nurse practitioners to learn best practices for the entire process of patient care, beginning with screening for hepatitis C and ending with curing the disease. Educational objectives include identification and diagnosis of patients with hepatitis C, potential medication side effects and interactions with other drugs and plans of action in the event of minor to severe internal organ damage.
“We look forward to expanding the number of locations where [hepatitis C virus] care is provided both through additional telemedicine partnerships and through training of new providers who can than provide access to HCV care in their own communities,” Dillingham wrote.
The hepatitis C virus infects the liver and causes inflammation. Those that suffer from acute hepatitis C experience symptoms including fatigue, loss of appetite, jaundice, hives and vomiting within the first few months following exposure. Chronic hepatitis C can develop decades later if the acute version is not treated, as is often the case, since many individuals do not develop symptoms early in the disease progression. According to the Centers for Disease Control and Prevention, 75 to 85 percent of patients develop chronic infections while a mere 15 to 25 percent clear the infection without treatment. Long-term viral attacks on the liver can cause scarring, liver cancer and failure. The CDC states that hepatitis C is one of the most common reasons for liver transplantation in the United States.
Transmission occurs through contact with the blood of a hepatitis C victim, and this commonly occurs when people share needles or other drug-use equipment. Personal hygiene items, sexual interactions and unsanitary instruments for tattoos and piercings contaminated with infected blood can spread the illness as well. Hepatitis C may also pass from mother to fetus.
One of the most important developments during the past few years that the Virginia HEPC emphasizes is making drugs that treat chronic hepatitis C available. Some of these treatments have up to a 95 percent cure rate. Dillingham mentioned, though, that many clinicians hesitate to prescribe these medications, as they doubt their effectiveness.
“The new medications that are being used are available nationwide — but there is an enormous lack of people who feel qualified to prescribe them — so they are not getting to the people who need them,” Dillingham said.
To further ensure everyone receives necessary medications, the Virginia HEPC details procedures for acquiring prescriptions for the insured and uninsured. Recently developed drugs may cost thousands of dollars, but according to Kemp-Knick, patients with Medicaid pay very little if anything out of pocket.
Treating people in the early stages of the disease may financially aid healthcare professionals as well. The Virginia HEPC program claimed clinics and hospitals will benefit from prescribing these medications and supporting patients throughout the regimen because they would save approximately $16.7 million in transplant costs.
Moreover, the course addresses social considerations in hepatitis C cases, such as the correlation between opioid and hepatitis C epidemics. According to Kemp-Knick, certain doctors and nurses refuse to accept patients that continue to use opioids or intravenously inject drugs. However, the Virginia HEPC encourages providers to tend to anyone who is hepatitis C positive.
“There are many people still using substances that have hepatitis C, and there is pushback from some doctors who do not want to see those people,” Kemp-Knick said. “We instruct them to treat everyone, though. We do not want people excluded because they consume drugs and alcohol.”
Implementing the policy to assist every hepatitis C victim becomes particularly critical in southwestern Virginia, Kemp-Knick said. According to data collected by the CDC, certain counties in southwest Virginia are disproportionately affected by the opioid epidemic compared to the rest of Virginia. In 2018, the CDC released a list of counties in the United States most vulnerable to HIV and/or hepatitis C outbreaks as a direct consequence of increased opioid use. Of the 220 counties listed, eight of them are located in Virginia, and all of them cluster near the southwestern tip of the state.
Not only does the Virginia HEPC aim to educate medical personnel, but they also look to create a network of providers. Rural areas often lack specialists equipped to manage disease complications. The hope is that fostering connections between remote counties with limited resources and medical experts will improve hepatitis C treatment across the state.
“We welcome the providers’ emails or their calls for advice and formal consultations,” Kemp-Knick said. “If they have a patient and have questions about how to treat them, we can help them, or if they have administrative questions, we can put them in touch with a nurse to help with that.”
As part of those efforts, Kemp-Knick mentioned that nine clinics in Virginia incorporated telemedicine into their treatment protocols. The Virginia HEPC program seeks to expand this infrastructure to new clinics statewide, in order to offer assistance to those who cannot easily reach doctors. This referral system extends to opioid doctors and primary care physicians, Kemp-Knick said, who can care for people with other health concerns.
“There are currently people traveling three to four hours to get treatment,” Kemp-Knick said. “We want everyone in Virginia, once they realize that there is available treatment for Hepatitis C, they can access that treatment locally.”
Kemp-Knick cited that the Virginia HEPC program has trained 36 providers, one of whom is currently practicing and another who will start shortly. Moving forward, Kemp-Knick and Dillingham intend to equip more clinics statewide with the resources to cure hepatitis C, and that, eventually, the disease will be eliminated from Virginia.