As colleges and universities across the country return their students to campus, many have established trackers or dashboards with the intention of being transparent about the number of COVID-19 cases in their communities. Compared to other universities in Virginia, U.Va.’s dashboard has many similar features — but also lacks some capabilities, such as not reporting the community’s COVID-19 positivity rate.
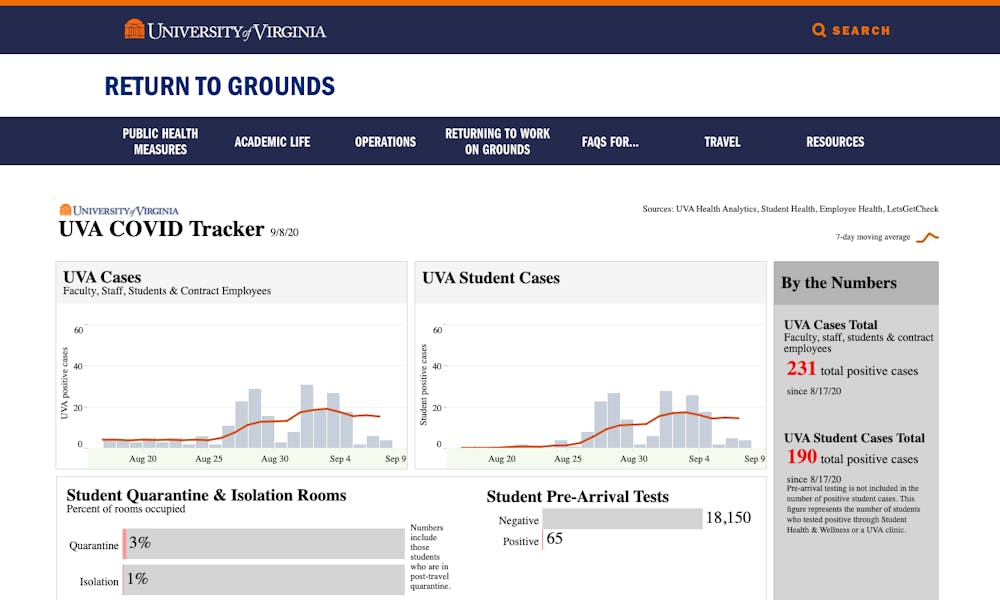
The dashboards from Virginia Tech, William and Mary, James Madison University, George Mason University and Virginia Commonwealth University all report the percentage of positive test results in their community. The University of Virginia does not — instead only reporting the number of positive COVID-19 cases in the community, which is currently 231. Percent positivity, a metric measuring how many tests out of the number performed are positive, can signal when virus spread in an area is out of control.
According to experts at Johns Hopkins, the percent positive is a crucial measure of viral spread.
“The percent positive is a critical measure because it gives us an indication how widespread infection is in the area where the testing is occurring — and whether levels of testing are keeping up with levels of disease transmission,” Doctors David Dowdy and Gypsyamber D’Souza wrote in an article for Johns Hopkins School of Public Health.
In a virtual Parent’s Town Hall held over the summer to discuss the University’s decision-making process in deciding whether to reopen Grounds, both University President Jim Ryan and Dr. Mitchell Rosner, the chair of the University of Virginia Department of Medicine, mentioned virus prevalence, which is often measured by percent positivity, as a metric that the University was paying attention to.
“One of the things that we’ve done is create a number of gating criteria that have to be met in order for us to feel that we can open up Grounds completely and do so safely,” Ryan said during the town hall. “These criteria look at things like the virus prevalence, our supply of PPE, our testing capacity, isolation and quarantine space.”
In a further explanation, Dr. Rosner explained the importance of viral prevalence in the area.
“You may have heard in the media that the WHO likes to show a number of about five percent where if numbers are below five percent, it’s a sign that the area has a handle on viral transmission,” Rosner said. “What we saw into late July and early August were viral positivity rates that approached seven-to-eight percent.”
As of press time, the current seven-day positivity rate in the Thomas Jefferson Health District, which includes the University of Virginia, Charlottesville and Albemarle County, is 7.1 percent.
Despite Ryan and Dr. Rosner’s statements suggesting the data is relevant, the University’s dashboard does not report percent positivity rates from tests conducted at the Student Health.
“To calculate an accurate positivity rate, you need to know the total number of tests being taken in a given community,” Wes Hester, deputy University spokesperson and director of media relations, said in an email statement to The Cavalier Daily. “Due to the range of testing services being used by U.Va. community members, there is no way to accurately calculate that total.”
When asked why other schools like James Madison University were able to clearly report percentage positivity data from their Student Health Center while the University of Virginia could not, Hester declined to speak to other school’s testing procedures.
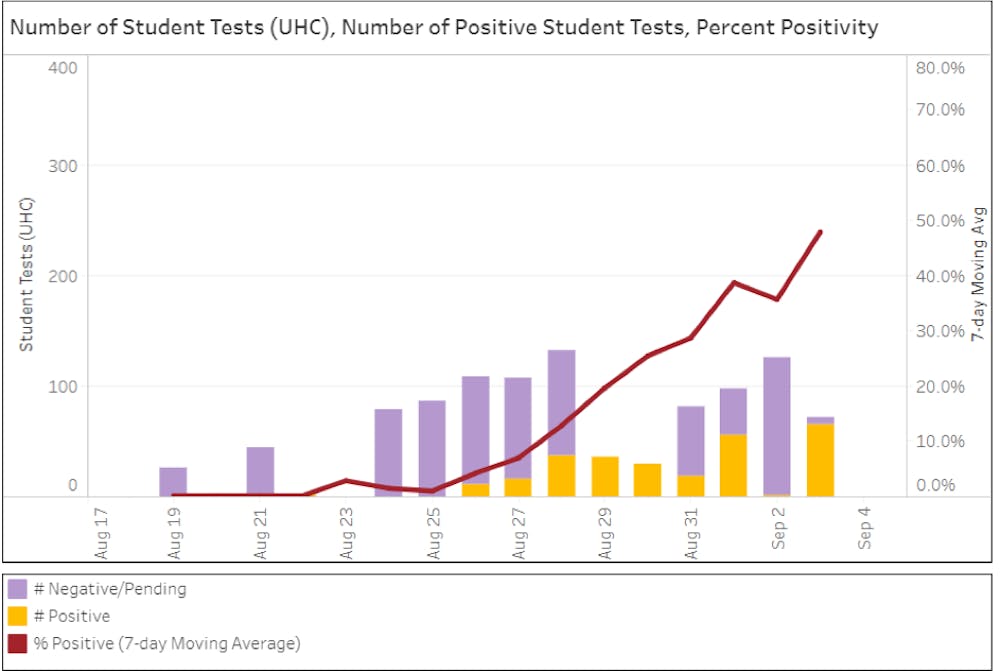
James Madison University announced it would suspend most in-person on Sept. 1, when the percentage of positive tests hit a seven-day moving average of 38.6 percent. (Courtesy James Madison University)
Like other Virginia schools, the University does not update its dashboard on weekends. U.Va.’s Student Health Center is only open for four hours on Saturday.
However, the University’s dashboard, which updates around 4:00 p.m. on weekdays, does display some crucial data that other schools do not.
For instance, the University clearly displays the percentage of quarantine and isolation beds that are occupied. In comparison, James Madison University displays the number of quarantine beds that are available on its dashboard. Virginia Tech’s dashboard shows the total number of students in quarantine.
According to a report from the Charlottesville Tomorrow, the University has created 1,500 quarantine beds.
U.Va.’s tracker also displays the number of hospitalizations per day as well as the average time it takes to get a test result returned, both of which are metrics that none of the other schools previously mentioned display.
“Our team monitors several viral transmission metrics to get a complete picture of both the state of the health district and on Grounds,” Hester said.
Hester added that the University is monitoring the rate of positive tests, despite that information not being displayed on the tracker.
“In addition [to the rate of positive tests], they are looking at case rates per 100,000, testing availability and turnaround times as well as other measures,” Hester said.
The University’s COVID-19 tracker does not currently report clusters, or groups of cases that appear linked.
At the University of North Carolina at Chapel Hill, a surge in reports of clusters in student housing likely factored into administrators to suspend in-person instruction. To date, UNC has reported 13 clusters — five or more cases of COVID-19 that are in close proximity — all linked to dormitories and Greek housing.
Hester suggested that the University may report cases in a similar manner.
“Emergency Management and public health officials are actively monitoring cases to identify outbreaks and will make determinations on appropriate communications with groups who are determined to be at risk of exposure,” Hester said.