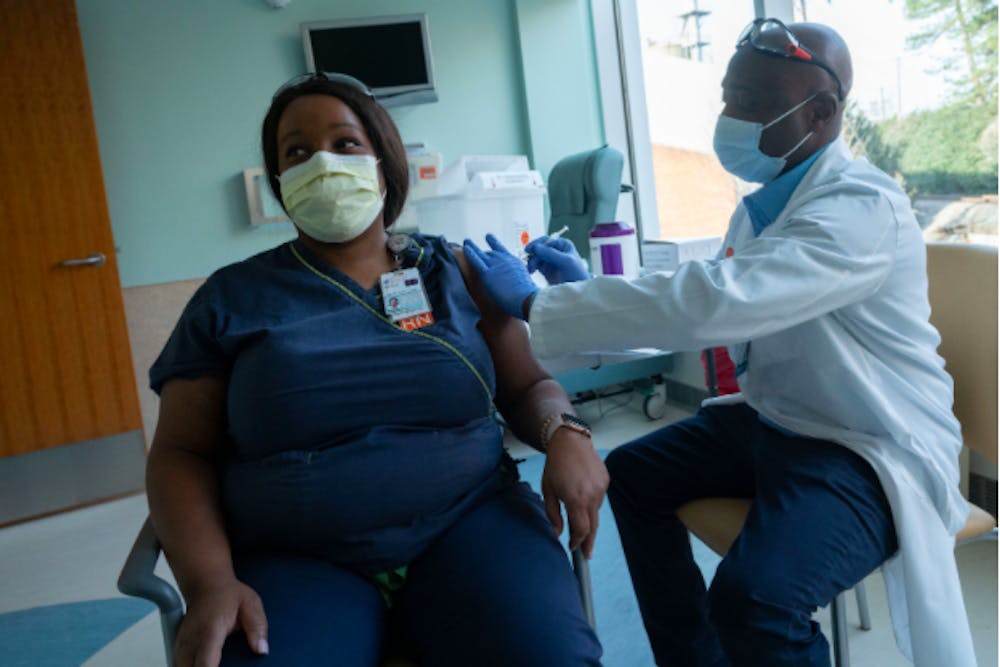
Starting Dec. 15, health officials have started administering COVID-19 to workers in the University Health System with 1,594 individuals being vaccinated within the first week and 4,000 individuals signed up for vaccination appointments. The first round of vaccinations are aimed towards physicians, nurses and support teams including environmental service workers, such as the custodial staff.
Wendy Horton, chief executive officer of the University Medical Center, has assisted in the hospital’s response throughout the COVID-19 pandemic and continues to play an administrative role during the vaccine distribution process. She spoke of the University Health System’s predicted timeline for the vaccination of all approximately 13,000 employees.
“Our goal as a health system is to try to vaccinate all of U.Va. Health by the end of March and that would include the second dose,” Horton said.
Currently, the University Health System has doses of both authorized vaccines with the first shipments containing 3,305 doses of the Pfizer vaccine and 2,500 doses of the Moderna vaccine. Both vaccines are based on the spike protein, also known as the S protein. The spike protein is what is used by the SARS-CoV-2 virus to enter cells in the human body. Both vaccines instruct cells to form a harmless piece of the spike protein, which allows the immune system to recognize a foreign protein and create an immune response. The building of this response results in the body’s new knowledge of how to protect against future infection.
The COVID-19 vaccines are not only characterized by their high efficacy — with Pfizer showing an efficacy rate of 95 percent and Moderna with a rate of 94.1 percent — but also by the time it took to produce both vaccines. Costi Sifri, director of hospital epidemiology in the University Health System, describes the unprecedented nature of the coronavirus's vaccine-developing process — from the identification of a novel pathogen and the publishment of its genome on Jan. 10, to the authorization of two highly efficacious only 11 months later.
“It's a couple years faster than what has been seen,” Sifri said. “Typically, it is under unique circumstances though however [that] we have a worldwide pandemic with high amounts of disease, and that actually has lent itself for the development of these vaccines because we could get to the endpoints and see if the vaccine was effective rather quickly compared to other vaccines that are in development.”
Throughout the first week of vaccinations at the U.Va. Hospital, the Pfizer vaccine was exclusively used due to its earlier arrival time, though the Moderna vaccine was delivered as of the morning of Dec. 23.
Since the Pfizer vaccine requires ultra cold freezing temperatures ranging from -70 degrees Celsius to -80 degrees Celsius, it has been shipped in larger quantities compared to the Moderna vaccine.
“Our current plan is to use the Pfizer vaccine until it's exhausted and then to switch over to the Moderna vaccine,” Sifri said.
The switchover to the Moderna vaccine occurred in the week of Dec. 28.
Of the University Health System workers that have received the vaccine thus far, no serious side effects have been reported, though local pain and discomfort have been a common symptom. Other reported symptoms during the observation period after vaccine administration included two people with nausea and one person with lightheadedness.
Sifri also described the excitement felt by the University Health community in response to the vaccine.
“I think we’ve been just incredibly gratified and excited about this opportunity to provide vaccines for our team members, and they’re certainly responding with their excitement as well,” Sifri said.
This excitement was echoed by Mesha Jones, a nurse within the University Health System who works on the wound care team as well as the critical care team and recently received the first dose of the COVID-19 vaccine. Her personal experience with COVID-19 is marked by the effort she has observed from her colleagues during her work and wound care in the South Tower, where the University emergency department is housed.
“Personally, I’ve just seen my colleagues and my friends work so hard, but staying positive although they are very tired and emotionally drained,”Jones said. “They still care for the patient like they were family or even [care] harder now because we have COVID, and families can’t be at the bedside.”
Jones researched and talked to trusted colleagues including Dr. Taison Bell, infectious disease physician and director of the University Intensive Care Unit, to address any concerns she had and to better understand the trials before deciding to take the COVID-19 vaccine.
“When I got the vaccine, I had no side effects,” Jones said. “As soon as I felt the vaccine go into my arm, it was like a burden that was lifted off my shoulders, and I felt hopeful for the next step.”
When asked about talking to others who are offered the opportunity to receive the vaccine soon, Jones hopes they realize the safety of taking it.
“It’s an individual’s decision to get the vaccine, but it’s safe, and everyone is being transparent about their [symptoms], or if they’re having any symptoms,” Jones said. “But it’s safe, and it’s our chance to move forward and get through this pandemic.”
Vaccinations are expected to continue being administered, focusing currently on healthcare providers, long term care facility residents and nursing home residents. Currently, the focus is not only on vaccinating University healthcare providers, but also those working in independent practice.