A team of U.Va. researchers, lead by Bijoy Kundu, Ph.D., earned a $1.9 million grant last week for a proposal to utilize medical imaging technologies to investigate the mechanism behind cardiac hypertrophy.
Kundu, asst. professor of radiology and medical imaging, is the principal investigator in this project. Kundu is working with Dr. Susanna Keller and Dr. Robert Carey from the Medical School and Dr. Heinrich Taegtmeyer from the University of Texas at Houston School of Medicine.
Cardiac hypertrophy is a condition in which the heart muscle stiffens and becomes enlarged. The heart eventually cannot sustain itself and fails. According to Keller, cardiac hypertrophy is an inevitable outcome in nearly all patients with high blood pressure.
According to Kundu, under normal conditions the heart uses fatty acids as fuel. However, when it undergoes stress it requires more fuel to function normally and looks for easy energy, increasing its usage of glucose.
However, though there is an abundance of glucose being taken up, the heart is not very efficient at utilizing the energy from the glucose—it is “starved amongst plenty,” Kundu said.
“The heart needs more fuel to function better but, at the same time the fuel that’s taken up is not efficiently used — it’s a futile cycle,” Keller said.
Identifying exactly how and when the switch from fatty acid metabolism to glucose metabolism occurs is the real challenge because of the overlap of various stages of the process, Keller said. “It’s a million dollar question.”
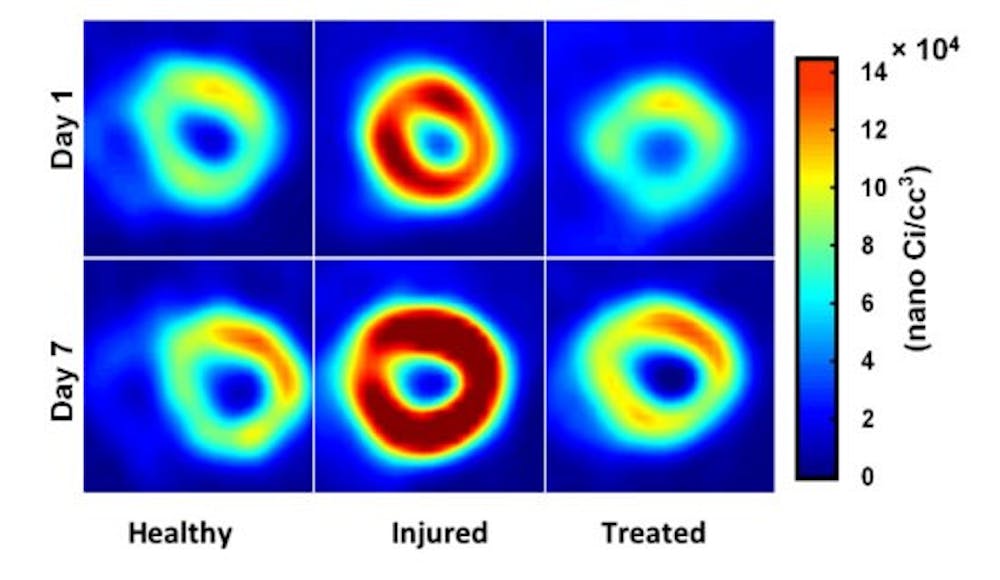
According to Kundu, his lab is uniquely equipped to tackle this problem: it is one of the few in the country that can do nuclear imaging, using a technique called Positron Emission Tomography to image live animal hearts.
However, imaging is just one aspect of the proposed research — Kundu and his collaborators plan to conduct metabolic and molecular analysis as well. Keller is working on the metabolic and molecular end, extracting proteins, metabolites and RNA to discern molecular differences between normal and hypertensive rats.
Once the researchers understand what is going on at the molecular level, they’ll be able to identify drugs that hit the right target.
Though there are currently no drugs specifically for cardiac hypertrophy, Kundu and his team plan to use the diabetes drug Metformin to make glucose use in the heart more efficient. Theirs is the first in vivo study to attempt to use Metformin in this way.
Therapeutic intervention is the ultimate goal, Kundu said.
“The idea would be [to be able to] just do a single PET scan and identify patients who are at more risk for progression toward the disease,” Kundu said. “It would be a kind of personalized medicine.”