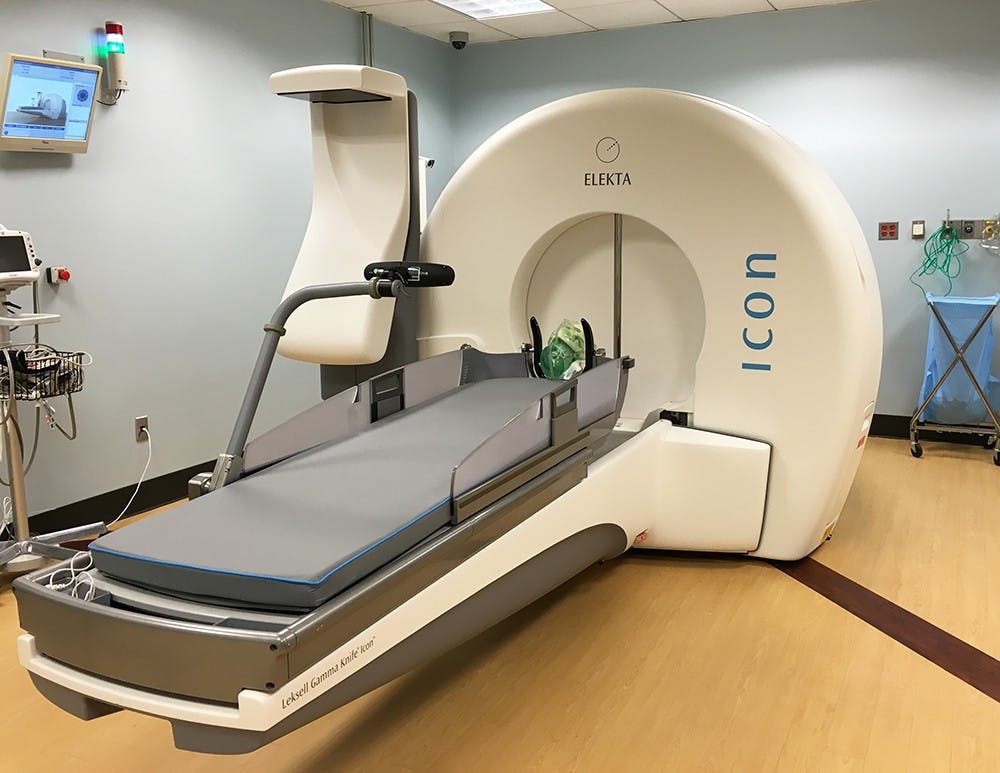
The Lars Leksell Gamma Knife Center in the University Health System, or UHS, was the first in the state, and one of the first in the country, to acquire Gamma Knife, a technology allowing completely noninvasive brain surgery.
Gamma Knife allows high energy gamma radiation to be used precisely within the brain to treat tumors, blood vessel abnormalities and pain disorders. This technology has been in use at UHS since 1989, and until very recently was only a minimally invasive approach — requiring the use of a frame that holds a patient’s head in place, which pierced the scalp and went into the skull to hold the head in place during the radiosurgery.
The newest iteration of the technology, Gamma Knife Icon, can be used completely non-invasively. This has been made possible by an on-board CT scanner and infrared tracking device, which track patient movements and allow the technology to correct for these movements.
Gamma Knife Center Director Dr. Jason Sheehan has worked with the technology for over 20 years.
“By using the Gamma Knife with the CT and infrared tracking, we can get precision down to 0.15 millimeters, so about a 10th of an inch … which is almost unheard of,” Sheehan said.
The ability to perform neurosurgery noninvasively, coupled with precision that is impossible with an open approach, makes this technology a preferred approach for patients.
“It’s going to be more safe for them, it tends to be more cost effective, they don’t have a long hospital stay,” Sheehan said. “The patient I operated on today with seven malignant brain tumors went home the same day, and she’s back to her normal activities and daily living.”
Sheehan said the technology will “permeate” the fields of neurosurgery and other surgical specialities, which are already trying to use more minimally invasive means to treat ailments.
Sheehan also noted this technology would not be possible without the strengths of many scientific disciplines — neuroradiology and the technologies it uses are based upon engineering and physics just as much as biology and medicine.
“There are no fewer than probably 12 different people that participate in every radiosurgical procedure with Gamma Knife,” Sheehan said. “Those people come from all different aspects of medicine and engineering and physics.”
One such team member is David Schlesinger, associate professor of radiation oncology who is a medical physicist on Sheehan’s team. Schlesinger’s role includes extensively testing and calibrating the Gamma Knife Icon, to ensure its safety for patients.
“So it’s everything from making sure the procedure is working to specification and doing quality assurance tasks to helping Dr. Sheehan shape the dose distribution,” Schlesinger said.
Sheehan believes the next step in treating brain tumors will be an interface between targeted brain operations such as those done by Gamma Knife Icon, and personalized medicine.
“There’s a synergistic effect … that when you couple medical therapies and you give them concurrently with Gamma Knife you suddenly get an effect that is more powerful than the Gamma Knife or the medical therapy alone,” Sheehan said. “I see this as being a merging of personalized medicine and targeted therapies, and that’s where I see the whole field evolving. The more focused, the more personalized the treatment for the patient the better.”